OCD vs. Hoarding
OCD vs. Hoarding
Hoarding used to be classified under Obsessive-Compulsive Disorder (OCD) as a symptom, but under the new edition of the Diagnostic and Statistical Manual of Mental Disorders or DSM-5, hoarding is now classified on its own under the category of “Obsessive Compulsive and Related Disorders”. OCD and Hoarding DSM-5 criteria compared below:
OCD:
The criteria for OCD as defined in the DSM-5:
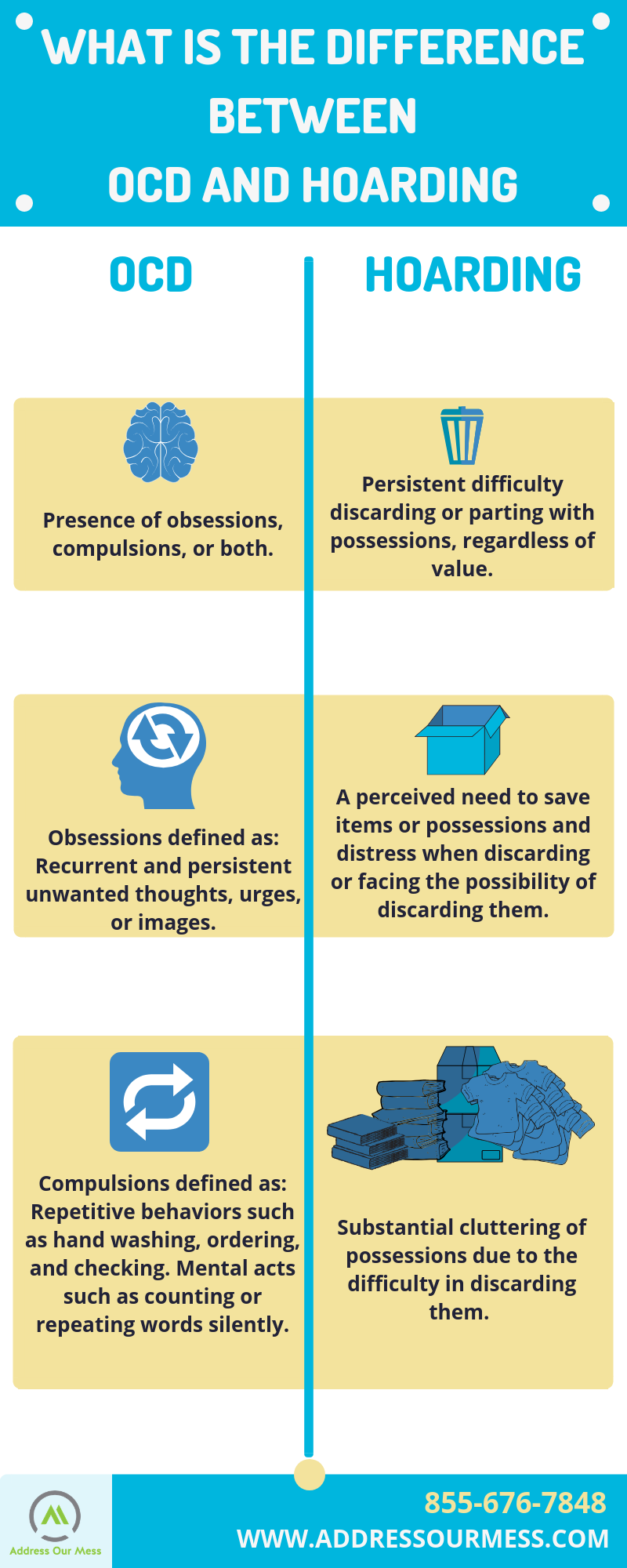
- Presence of obsessions, compulsion, or both:
Obsessions are defined by (1) and (2):
- Recurrent and persistent thoughts, urges, or images that are experienced, at some time during the disturbance, as intrusive and unwanted, and that in most individuals cause marked anxiety or distress.
- The individual attempts to ignore or suppress such thoughts, urges, or images, or to neutralize them with some other thought or action (i.e., by performing a compulsion).
Compulsions are defined by (1) and (2):
- Repetitive behaviors (e.g., hand washing, ordering, checking) or mental acts (e.g., praying, counting, repeating words silently) that the individual feels driven to perform in response to an obsession or according to rules that must be applied rigidly.
- The behaviors or mental acts are aimed at preventing or reducing anxiety or distress, or preventing some dreaded event or situation; however, these behaviors or mental acts are not connected in a realistic way with what they are designed to neutralize or prevent, or are clearly excessive.
Note: Young children may not be able to articulate the aims of these behaviors or mental acts.
- The obsessions or compulsions are time-consuming (e.g., take more than 1 hour per day) or cause clinically significant distress or impairment in social, occupational, or other important areas of functioning.
- The obsessive-compulsive symptoms are not attributable to the physiological effects of a substance (e.g., a drug of abuse, a medication) or another medical condition.
- The disturbance is not better explained by the symptoms of another mental disorder (e.g., excessive worries, as in generalized anxiety disorder; preoccupation with appearance, as in body dysmorphic disorder; difficulty discarding or parting with possessions, as in hoarding disorder; hair pulling, as in trichotillomania [hair-pulling disorder]; skin picking, as in excoriation [skin-picking] disorder; stereotypies, as in stereotypic movement disorder; ritualized eating behavior, as in eating disorders; preoccupation with substances or gambling, as in substance-related and addictive disorders; preoccupation with having an illness, as in illness anxiety disorder; sexual urges or fantasies, as in paraphilic disorders; impulses, as in disruptive, impulse-control, and conduct disorders; guilty ruminations, as in major depressive disorder; thought insertion or delusional preoccupations, as in schizophrenia spectrum and other psychotic disorders; or repetitive patterns of behavior, as in autism spectrum disorder).
Hoarding:
The criteria for Hoarding as defined in the DSM-5:
- Persistent difficulty discarding or parting with possessions, regardless of their actual value.
- This difficulty is due to a perceived need to save the items and to distress associated with discarding them.
- The difficulty discarding possessions results in the accumulation of possessions that congest and clutter active living areas and substantially compromises their intended use. If living areas are uncluttered, it is only because of the interventions of third parties (e.g., family members, cleaners, authorities).
- The hoarding causes clinically significant distress or impairment in social, occupational, or other important areas of functioning (including maintaining a safe environment for self and others).
- The hoarding is not attributable to another medical condition (e.g., brain injury, cerebrovascular disease, Prader-Willi syndrome).
- The hoarding is not better explained by the symptoms of another mental disorder (e.g., obsessions in obsessive-compulsive disorder, decreased energy in major depressive disorder, delusions in schizophrenia or another psychotic disorder, cognitive deficits in major neurocognitive disorder, restricted interests in autism spectrum disorder).
Hoarding and OCD Causes
It's not entirely clear what causes OCD and Hoarding however there are some research that has linked genetics, brain functionality, and when it comes to hoarding there have been links to a traumatic event. Brain functionality could mean damaged or impaired functionality either from illness, drugs, or physical damage.
The Difference between OCD and Hoarding
OCD is having reoccurring thoughts, urges, or images and having a compulsion to try to minimize or remove them whereas hoarding is having not an obsession with the items but rather having difficulty in letting things go. OCD compulsions such as hand washing, counting, or repetitive tasks to minimize or reduce the persistent thoughts or urges can result in disruptions to daily life and may cause avoidance of social situations. Hoarding results in clutter due to the difficulty in letting things go which can affect the health of the home environment and avoidance of having anyone entering the home.
What is Behavioral Therapy?
Behavioral Therapy is therapy to treat mental disorders. The therapy is used to identify and change self-destructive or unhealthy behaviors by changing some behaviors and creating new behaviors through activities and exercises. One of the most common forms is "cognitive behavioral therapy" which combines cognitive therapy with behavioral therapy which uses problem solving to meet goals of changing patterns of thinking and behaviors.
Therapist List:
- ABCT – Association for Behavioral and Cognitive Therapies
http://www.findcbt.org/xFAT/index.cfm - ADAA – Anxiety and Depression Association of America
https://members.adaa.org/search/custom.asp?id=4685 - IOCDF – International OCD Foundation
https://iocdf.org/find-help/